Enhancing Intraoperative Teaching in Anesthesiology: Theory, Strategies, and Practical Implementation
Mona Hedayat, MD
Published July 3, 2025 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
Intraoperative teaching is one of the most powerful, yet often underutilized, tools in anesthesiology education. The operating room offers real-time decision-making, evolving physiology, and critical moments that are ripe for learning, but the demands of clinical care, documentation, and time pressures often push teaching to the background. This article explores the principles behind effective intraoperative teaching, shares ideas for making these teaching moments more visible to residents, and offers practical strategies to integrate it seamlessly into workflow.
The Theory Behind Intraoperative Teaching
Intraoperative teaching lives at the intersection of clinical care and experiential learning. Unlike classroom-based education, the operating room provides a high-stakes, high-fidelity environment where decisions are made in real time. This makes it a prime setting for applying situated learning theory, which emphasizes learning that occurs in context through observation, participation, and collaboration.
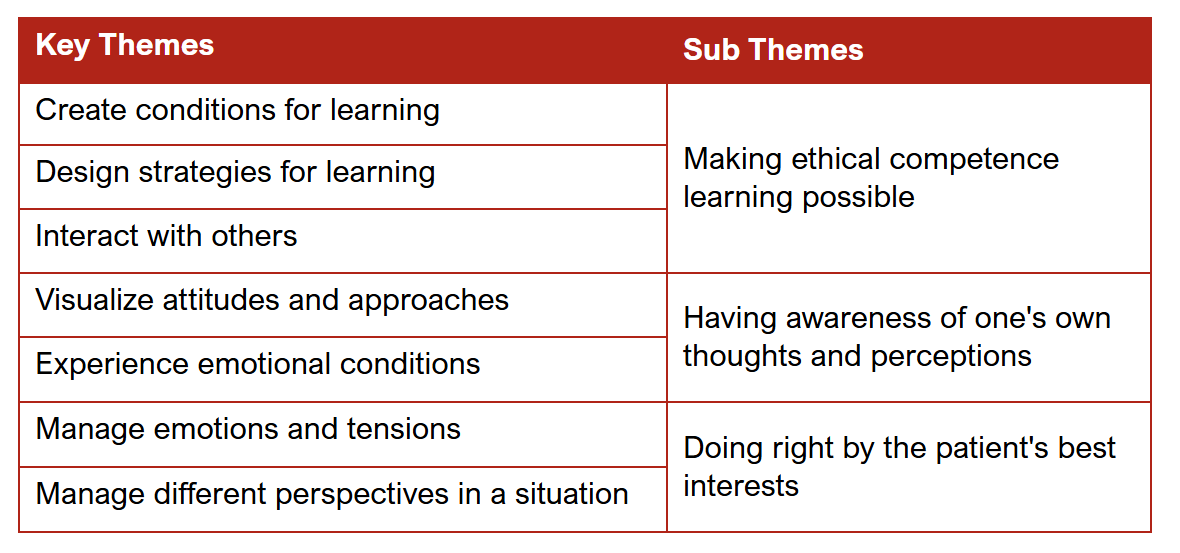
TABLE 1
Curriculum themes
Making Teaching Moments Visible
In the OR, teaching often goes unnoticed when clinical decisions aren’t explained. Faculty may believe they’re teaching through role modeling, but without verbalizing their reasoning, residents miss the learning opportunity. A simple fix: signpost teaching with cues like “Let me explain why I’m doing this…” or “Quick teaching point…”. These phrases highlight key moments and prompt residents to engage. Micro-reflection prompts like “What if the pressure hadn’t improved?” or “What surprised you?” take seconds but deepen learning and reveal thought processes. Teaching doesn’t require more time rather just intentional language to make it visible.
Using EBM at the Point of Care
Evidence-based medicine can feel distant in the OR, but real-time tools like OpenEvidence make it accessible. Faculty can model how to quickly find and apply evidence during cases, reinforcing critical thinking and lifelong learning. Even brief references to guidelines or studies help residents understand clinical reasoning. Asking them to follow up on a question post-op extends the learning. Incorporating EBM in real time fosters a culture where decisions are data-driven, not just based on intuition.
Bringing PBLD-Style Teaching into the OR
PBLDs (structured, case-based discussions) can be adapted for the OR to encourage active learning. Treat each case like a living PBLD by asking scenario-based questions, e.g., “If this patient had a difficult airway, how would your plan change?”
Even short prompts stimulate critical thinking beyond the current case. Faculty can keep a mini-bank of case scenarios to use pre-, intra-, or post-op (e.g., “How would you manage Eliquis in a 70-year-old for lap chole?”). One PBLD-style question a day can shift intraoperative teaching from passive observation to active participation, without adding time.
Practical Tips for Faculty: Making Intraoperative Teaching Part of the Routine
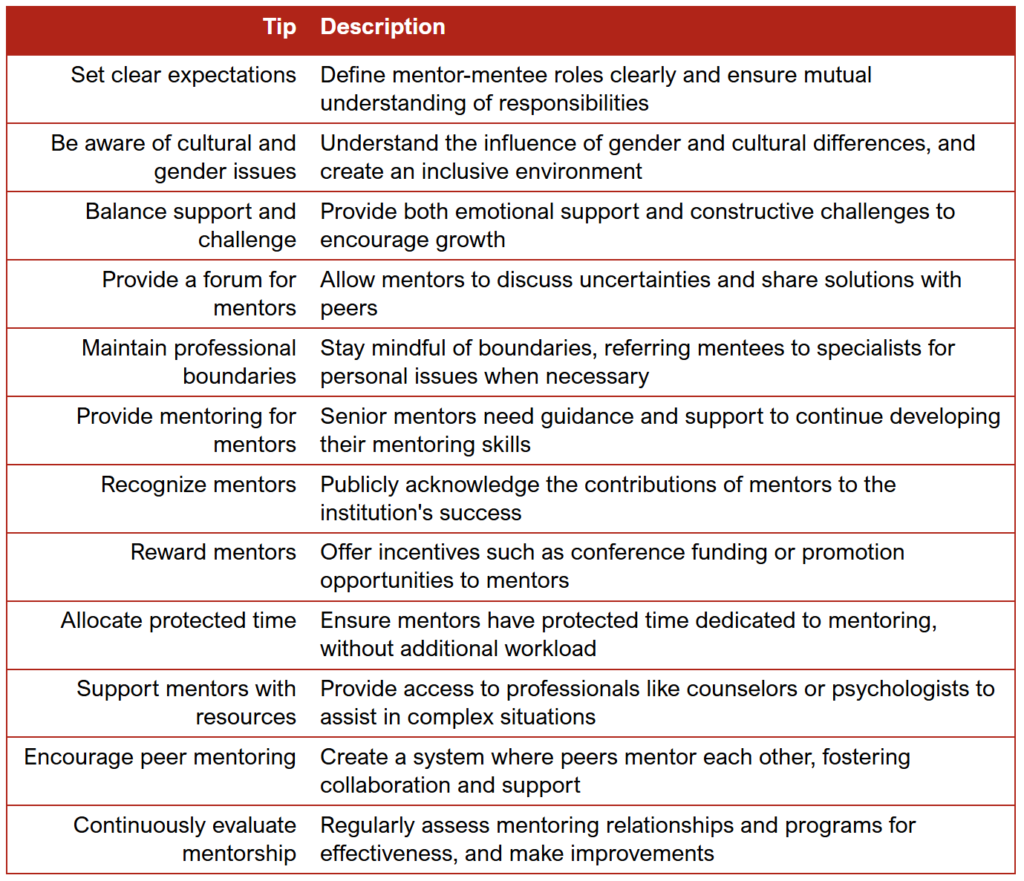

Conclusion: Shaping a Culture of Teaching
Intraoperative teaching does not need to be formal, lengthy, or disruptive to clinical care. When approached intentionally, it can be woven seamlessly into the operative workflow, transforming routine cases into valuable educational experiences. Some of the most effective teaching occurs in brief, unscripted exchanges: a narrated rationale, a thoughtfully posed question, or a moment of guided reflection.
