Basics of Scalp Block
Robina Matyal, MD, Rakalin Andrey, MD
Published July 3, 2025 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
Scalp block is a simple, straightforward technique that can be helpful in providing anesthesia in awake craniotomy or analgesia for postoperative neurosurgical pain. Although ultrasound is not currently used to perform the blocks, it is a must to describe them due to their clinical relevance and for completion.
Pain after neurosurgical procedures with craniotomy presents a challenge for pharmacologic management. Greater than 2/3 of patients undergoing craniotomy report moderate to severe postoperative pain. Intense pain in the postoperative period is associated with hemodynamic instability (with hypertension and tachycardia), psychomotor agitation, increased oxygen consumption, and activation of the stress response.
Non-steroidal anti-inflammatory drugs alter normal platelet function and prolong bleeding times. They are relatively contraindicated in neurosurgical procedures, especially in patients at high risk of bleeding (aneurysm repair, arteriovenous malformation resections, hematoma evacuation, etc.). On the other hand, opioids are effective in managing post-craniotomy pain, but present additional problems in the neurosurgical patient.
Opioid drugs are associated with postoperative nausea and vomiting, which can increase intracranial pressure. Additionally, they can produce respiratory depression, with lowering of the respiratory rate and possible hypoxemia and hypercapnia; this in turn can lead to sustained increases in intracranial pressure. Further, awake craniotomy is being performed more and more frequently, and these procedures require the anesthesiologist to administrate lower doses of sedating agents.
Advantages of Scalp Block
The advantage of scalp block when compared with surgical incision infiltration with local anesthetic is its longer duration of action and better attenuation of the hemodynamic responses associated with pinning and surgical incision. Scalp block has also been shown to decrease the amount of rescue pain medication required and increase the time between the end of surgery and the first request for postoperative analgesics. When compared to standard analgesic management, scalp block has demonstrated lower pain scores for up to 48 hours after surgery.
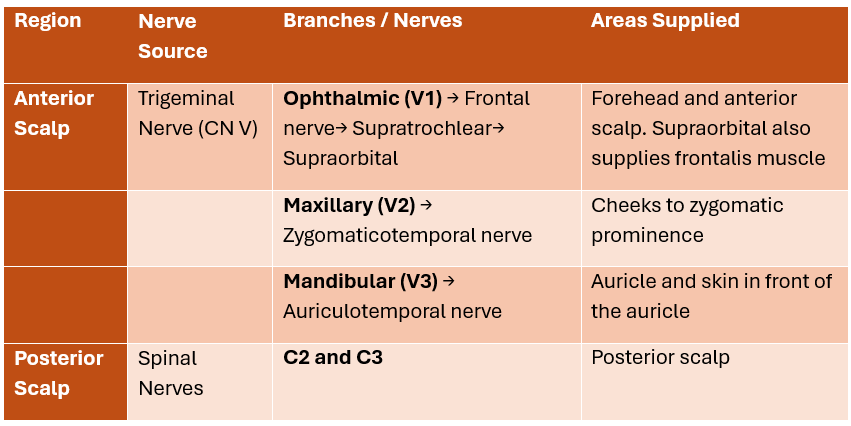
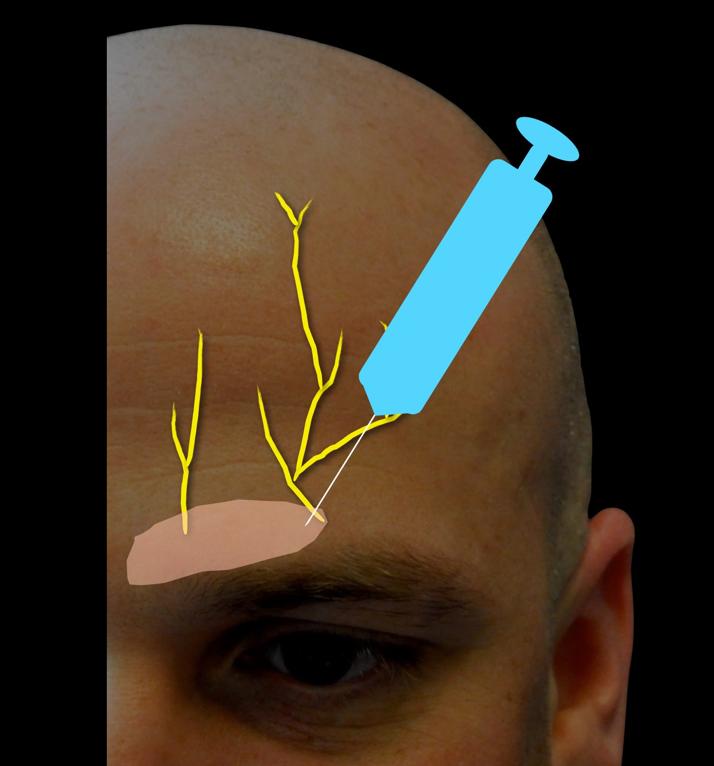
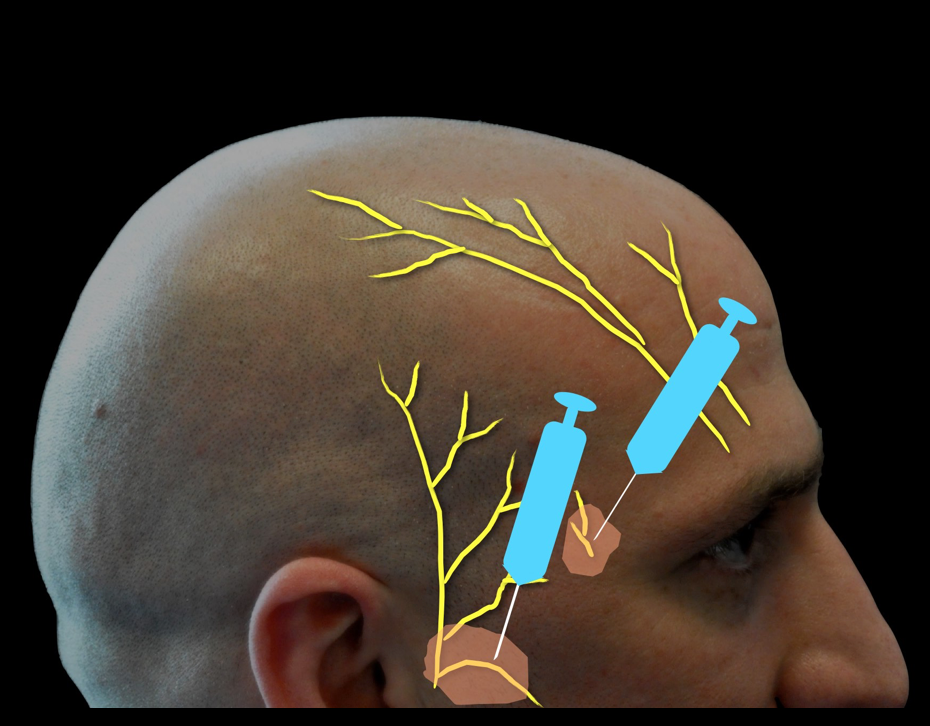
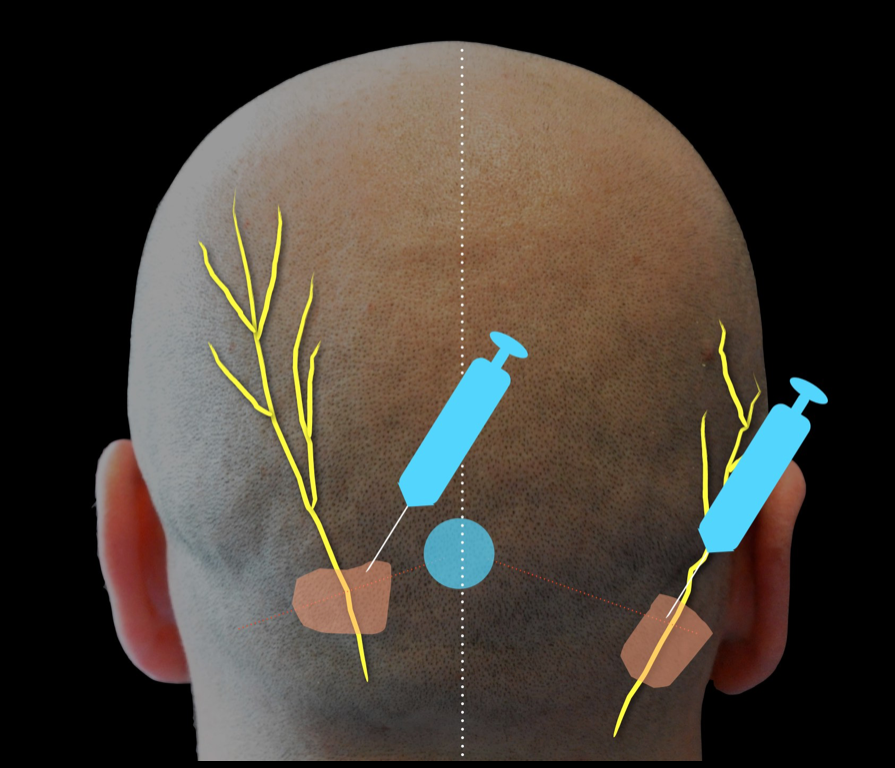
Preparation
This block can be performed on the awake patient in a sitting or supine position. On an anesthetized patient the supine position is more commonly used. The head may be rotated to provide better access for injection of the auriculotemporal, lesser occipital, and greater occipital nerves. The block is associated with moderate discomfort due to the multiple injections required, so sedation and analgesia can be administered, preferably with short acting agents. This is particularly important in the patient who will undergo awake craniotomy. The skin is disinfected with chlorhexidine solution. Be careful to prevent the solution from contacting the patient’s eyes, as this may cause injury.
Technique
- Start: Prepare Equipment and Patient
- Gather syringes (2-5 ml) with local anesthetic, 25G needles
- Choose local anesthetic (e.g., 0.25-0.5% Bupivacaine with epinephrine 1:200 000)
- Anesthetized, supine patient; disinfect skin (avoid eyes)
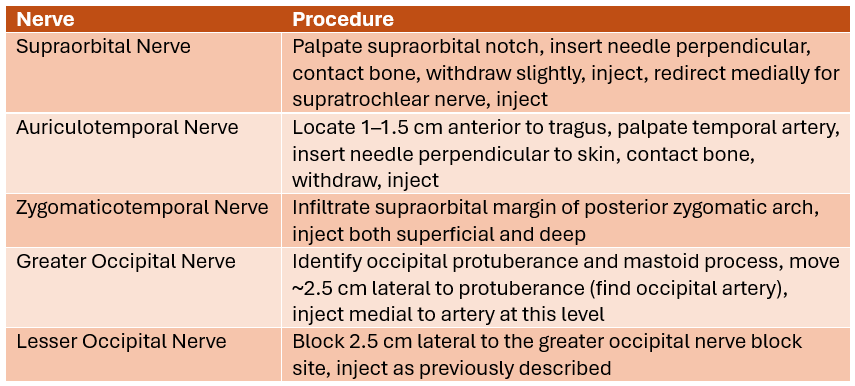
Complications
Intravascular injection and local anesthetic toxicity are the most common complications associated with this block. To avoid these, use the lowest effective dose of local anesthetic and identify the temporal and occipital arteries prior to injection. Hematoma can also occur due to injury of these arteries. Subarachnoid injection of local anesthetic has been reported during lesser occipital nerve block on a patient that underwent previous retromastoid craniotomy. Facial nerve paralysis has not been reported, although the proximity of the facial nerve to the sensory nerves of the scalp could theoretically make this complication possible.
Contraindications
Scalp block is not recommended if there is a bone defect in the cranium, for example resulting from prior craniotomy. As with other block techniques, coagulopathy and infection at the needle insertion site are contraindications to this procedure. Identify the occipital and temporal arteries before injection, in order to minimize the risk of unintentional intravascular injection or hematoma formation. When cleaning the intended injection site, take care to avoid depositing cleaning solution in the patient’s eyes. Intravascular injection or absorption of local anesthetic with epinephrine could cause hypertension. Please monitor accordingly. Avoid overly sedating or long- acting drugs in patients undergoing awake procedures.
REFERENCES
1. Ortiz-Cardona J, Bendo AA. Perioperative pain management in the neurosurgical patient. Anesthesiol Clin 2007; 25(3):655-74, xi.
2. Lai LT, et al. Perioperative pain management in the neurosurgical patient. Anesthesiol Clin 2012; 30(2):347-67
