The Use of Hand Motion Metrics and Eye Tracking for Objective Evaluation of Procedural Skills Development in Ultrasound-Guided Procedures
Jacqueline Hannan, PhD
Published July 3, 2025 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
Ultrasound-guided procedures are core competences in anesthesiology, but their technical complexity can pose challenges for training and introduce patient safety threats [1,2]. All ultrasound-guided procedures have common motion and require needle tracking in the three-dimensional space for precision and to avoid causing structural harm. Currently, training in these procedures relies on subjective assessment and remains highly variable, leading to inconsistent performance and increased complication rates. Additionally, common educational approaches focus on a time-based learning model with an assumption of proficiency after a specific amount of exposure, failing to account for the diverse learning trajectories of each trainee. An alternative competency-based approach with repeated practice in a safe setting ensures a more equal skill level among trainees when compared to a timebased approach [3].
In teaching a variety of anesthesia procedural skills, adding simulation training has resulted in improved performance, a reduction in needle passes, and decreased complications [4,5]. However, these skills are often trained with a fixed number of practice sessions in a calm setting, neglecting the need to perform the procedure with divided attention in an environment with distractions, such as beeping alarms, talking, and multitasking [6]. In surgical programs, overtraining residents beyond proficiency has enhanced trainee performance and multitasking ability [7,8]. These results from training laparoscopic surgery skills provide evidence for conducting extensive pre-clinical training to support patient safety and effective learning experiences in the clinical environment, along with improved retention of trained skills. Pairing this training approach with the implementation of objective measures to quantify proficiency can help track the advancement of trainees’ procedural skills towards expert-level performance.
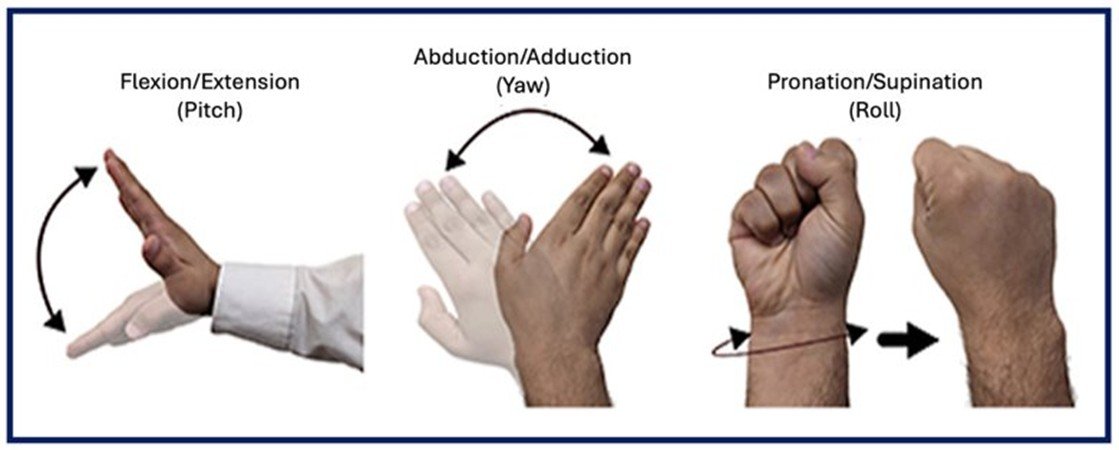
FIGURE 1
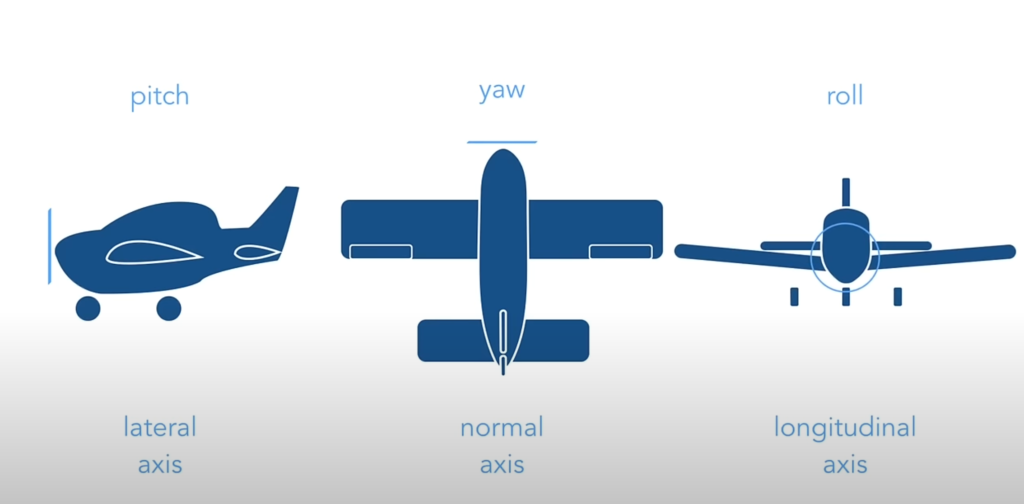
Hand motion can be defined and quantified using aircraft principal axes, measuring the angular motion along the cartesian coordinate frame as pitch, yaw, and roll [9].
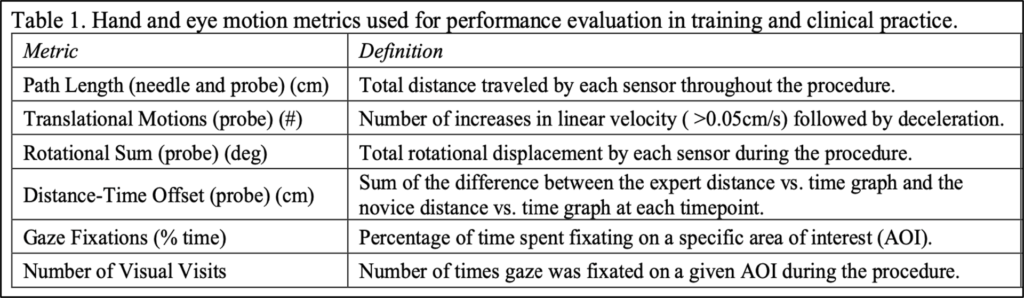
Biomechanical analysis of hand motion has emerged as a promising method for objectively evaluating procedural skill, and results show that improving hand motion metrics (reduced path length, fewer movements, and continuous needle tip tracking) correlate with higher visual assessment scores across various procedures [9–13]. At Beth Israel Deaconess Medical Center (BIDMC), researchers have demonstrated the feasibility of using hand motion metrics to differentiate between novice and expert operators and evaluate for improvement in echocardiography procedures and radial artery access [12,13]. In addition to hand motion analysis, eye tracking has been leveraged in medical training to provide context about the operator’s attention, giving a first-person perspective to support technique improvement [14]. By leveraging these technologies, objective measures can be derived to perform anesthesia procedural skills with expert-level competency.
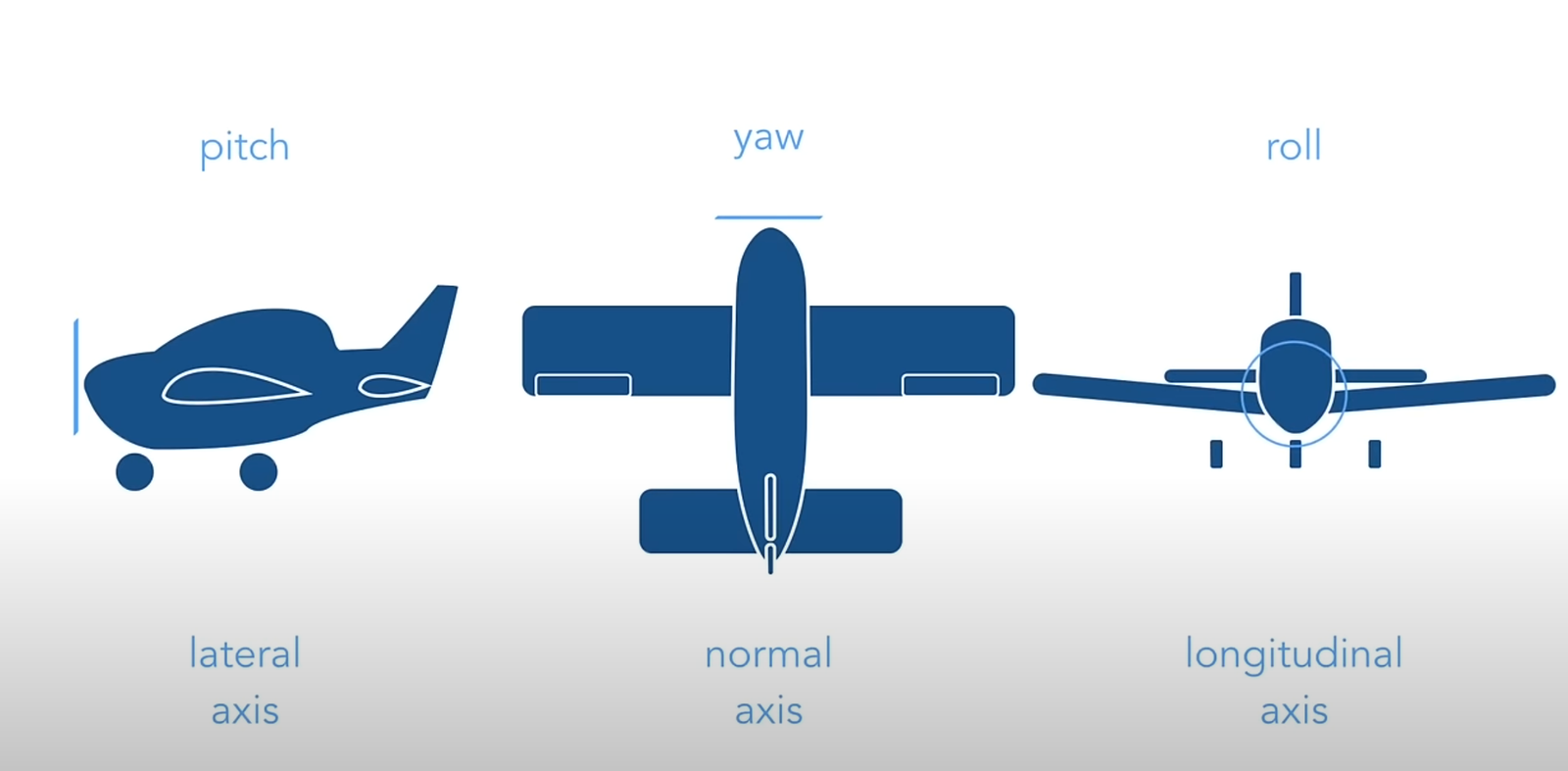
FIGURE 2
Aircraft principal axes
REFERENCES
[1] J. P. Corcoran et al., “Ultrasound-guided procedures,” Thoracic Ultrasound, vol. 79, p. 226, 2018.
[2] B. Teja et al., “Complication rates of central venous catheters: a systematic review and meta-analysis,” JAMA Internal Med., vol. 184, no. 5, pp. 474–482, 2024.
[3] M. V. Pusic et al., “Learning curves in health professions education,” Acad. Med., vol. 90, no. 8, pp. 1034–1042, 2015.
[4] E. J. Oh et al., “Simulation-based training using a vessel phantom effectively improved first attempt success and dynamic needle-tip positioning ability for ultrasound-guided radial artery cannulation in real patients: an assessor-blinded randomized controlled study,” PloS One, vol. 15, no. 6, p. e0234567, 2020.
[5] J. Tokumine et al., “Outcome-based simulation training for ultrasound-guided central venous catheter placement: clinical impact on preventing mechanical complications,” BMC Med. Educ., vol. 25, no. 1, p. 131, 2025.
[6] M. R. Endsley, “Toward a theory of situation awareness in dynamic systems,” Hum. Factors, vol. 37, no. 1, pp. 32–64, 1995.
[7] J. M. Poolton et al., “Multitask training promotes automaticity of a fundamental laparoscopic skill without compromising the rate of skill learning,” Surg. Endosc., vol. 30, no. 9, pp. 4011–4018, 2016, doi: 10.1007/s00464-015-4713-9.
[8] R. Castillo, J. Alvarado, P. Moreno, P. Billeke, C. Martínez, J. Varas, and N. Jarufe, “Validation of a visual-spatial secondary task to assess automaticity in laparoscopic skills,” J. Surg. Educ., vol. 75, no. 4, pp. 1001–1005, Jul.–Aug. 2018, doi: 10.1016/j.jsurg.2017.11.007.
[9] J. L. Weinstein et al., “Evaluation of technical performance of ultrasound-guided procedures through hand motion analysis: an exploration of motion metrics,” J. Vasc. Interv. Radiol., vol. 34, no. 8, pp. 1337–1344, 2023.
[10] R. Matyal et al., “Evaluation of the quality of transesophageal echocardiography images and verification of proficiency,” Echo Res. Pract., vol. 5, no. 3, pp. 89–95, 2018.
[11] R. Matyal et al., “Manual skill acquisition during transesophageal echocardiography simulator training of cardiology fellows: a kinematic assessment,” J. Cardiothorac. Vasc. Anesth., vol. 29, no. 6, pp. 1504–1510, 2015.
[12] R. Matyal, J. Mitchell et al., “Simulator-based transesophageal echocardiographic training with motion analysis: a curriculum-based approach,” Anesthesiology, vol. 121, no. 2, pp. 389–399, 2014.
[13] J. L. Weinstein, F. El-Gabalawy, A. Sarwar et al., “Analysis of kinematic differences in hand motion between novice and experienced operators in interventional radiology: A pilot study,” J. Vasc. Interv. Radiol., [Online]. [Early Access – full details such as volume and year not provided].
[14] G. A. Wright et al., “Eye-tracking technology to determine procedural proficiency in ultrasound-guided regional anesthesia,” J. Educ. Perioper. Med., vol. 24, no. 1, p. E684, Jan. 2022.