Implementation of VR Training for Neuraxial Pain Procedures among Anesthesia Interns, Residents and Pain Fellows
Adil Al-Karim Manji, MD, Shiri Savir, MD
Published July 3, 2025 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
Reimagining Neuraxial Training in the Age of Immersive Technology
In the hands of an anesthesiologist, a neuraxial needle demands both precision and deep anatomical knowledge. From epidurals to spinal blocks and pain procedures, these techniques are central to our field—but they come with a steep learning curve, especially in the high-pressure OR. Despite years of apprenticeship-style training and advanced manikins, something crucial has been missing: the ability to truly “see” and “feel” spinal anatomy before working on real patients. Virtual Reality (VR) is changing that. Already proven in surgery, radiology, and regional anesthesia, immersive VR enhances spatial understanding and builds confidence. For neuraxial training, it may be a game-changer allowing learners to explore 3D spinal anatomy from every angle, safely and interactively.
But VR alone isn’t enough. What if we could bring live mentorship, peer discussion, and real-time Q&A into the virtual space? That’s exactly what our team set out to do.
The Neuraxial Masterclass: A Shared Virtual Classroom
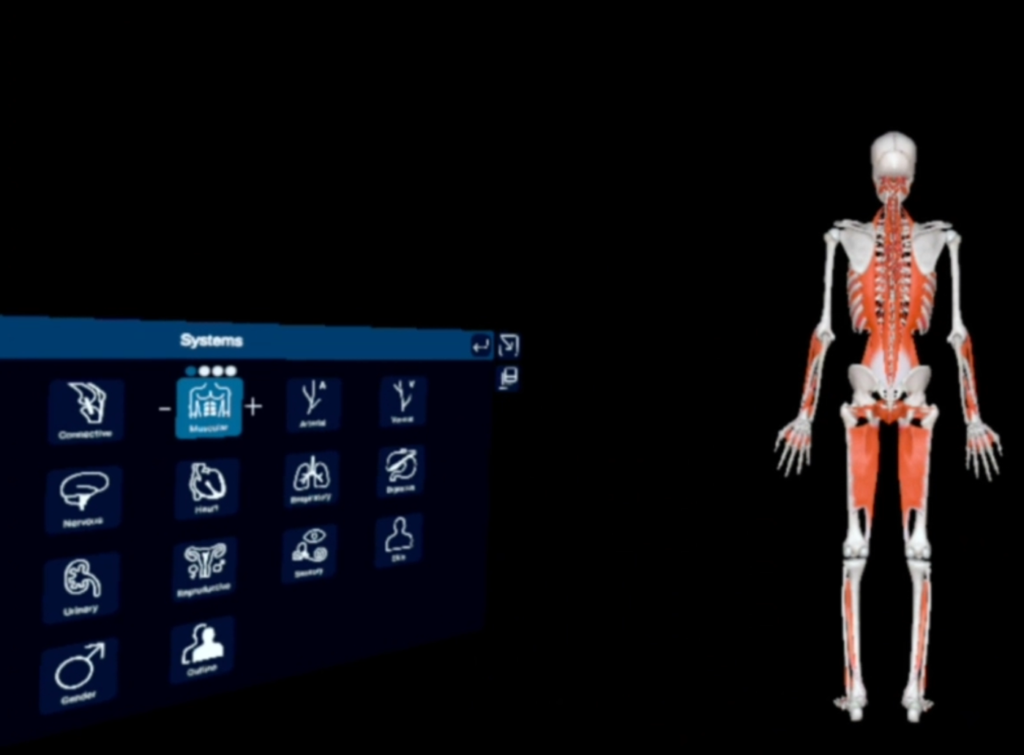
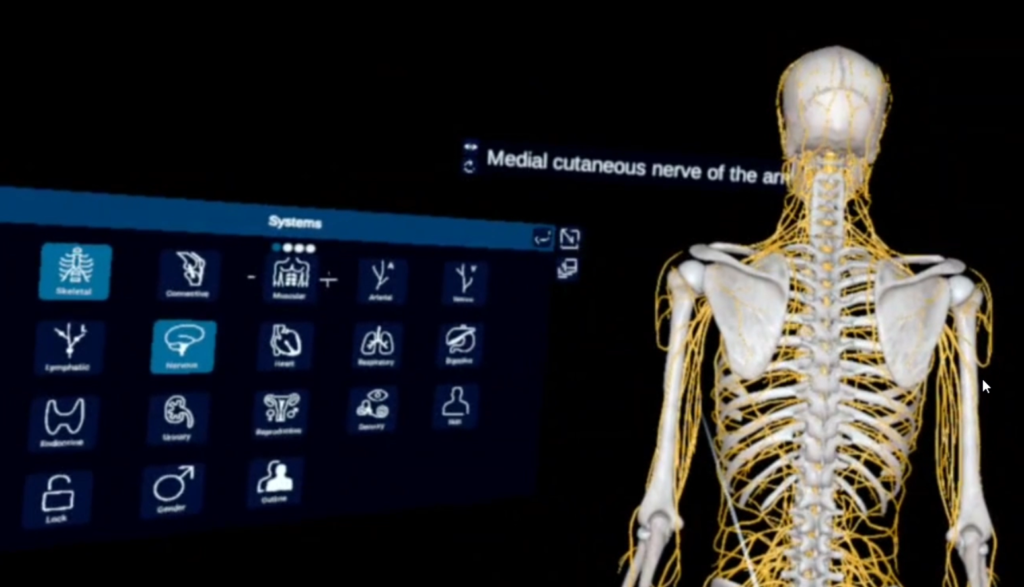
To address this gap, we developed a multi-institutional, instructor-led VR “neuraxial masterclass” for anesthesiology residents and fellows. Using the 3D Organon platform and Meta Quest headsets, learners entered a shared virtual space to explore spinal anatomy and practice procedures together. Guided by faculty in real time, participants identified landmarks, observed demonstrations, and received immediate feedback during hands-on virtual practice. The result was a fully immersive experience that combined the realism of simulation with the interactivity of traditional teaching. The masterclass began with a guided walkthrough of the spine. Trainees examined vertebrae from cervical to sacral levels, isolated structures like the ligamentum flavum and interlaminar space, and used cross-sectional views to visualize the epidural and subarachnoid compartments. They compared lumbar to thoracic anatomy and explored pathological variations like stenosis or hypertrophy, details often difficult to appreciate in cadavers or textbooks.
Needle to Virtual Skin
Next, participants used VR controllers to practice midline and paramedian approaches for thoracic and lumbar epidurals, and cervical interlaminar injections. They observed peers, received real-time feedback, and repeated procedures safely and risk-free.The session concluded with a debrief and Q&A, where instructors reinforced key concepts and encouraged reflection on real-world experiences.


Measuring Impact
Participants completed pre- and post-session assessments focused on core anatomy and procedural principles. They also filled out satisfaction surveys evaluating usability, realism, and educational value. Open-ended feedback captured their impressions of the instruction, visual-spatial immersion, and peer interaction within the virtual operating room.
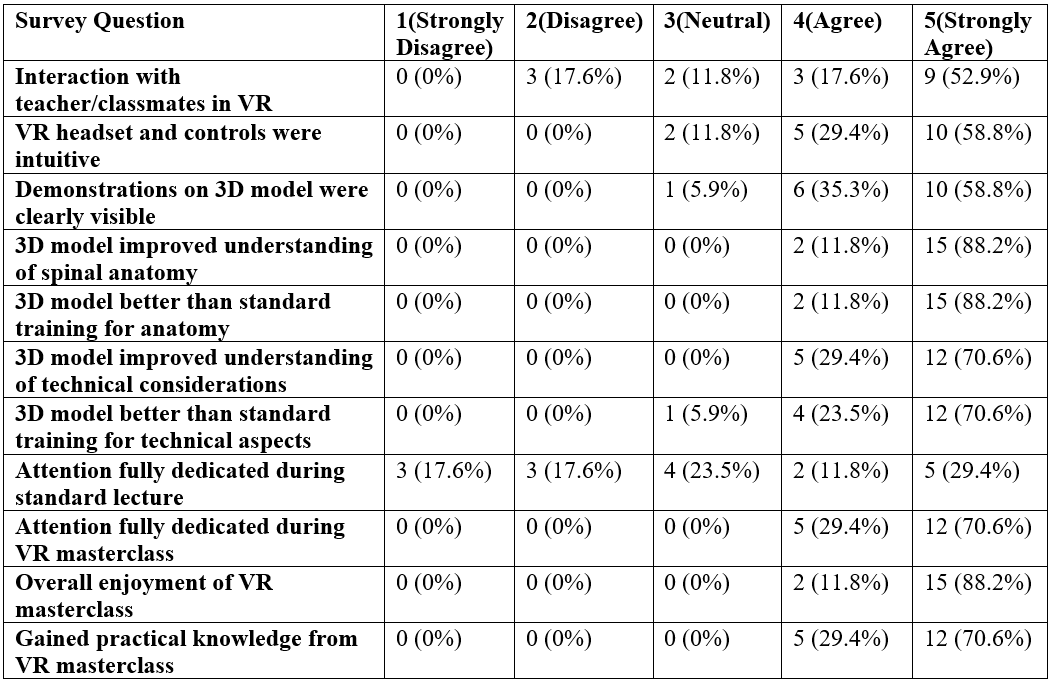
TABLE 1
Survey Results
A total of 34 participants attended the VR masterclass across three sessions (one excluded due to technical issues), including 6 medical students/interns, 17 residents, 7 fellows, and 4 attending physicians. Of these, 21 participants (3 medical students/interns, 12 residents, and 6 fellows) completed both pre- and post-session knowledge assessments. The average pre-test score was 53.2%, which increased to 77.1% post-session, reflecting a mean knowledge gain of 23.9%. Eighteen participants (90%) demonstrated improvement, with several achieving gains of over 40%. Only two showed a decline in post-test scores. In addition, 17 participants completed the post-session survey, which included a mix of learners across all training levels.
From Pilot to Platform
This pilot shows the feasibility and potential of multi-user VR as a scalable, engaging tool for teaching complex spatial skills in anesthesiology. By combining immersive visualization with instructor-led guidance, we preserved the human element of learning while enhancing anatomical understanding. As VR evolves, so must our teaching. It’s more than simulation. It’s a new, social and spatial way to learn. Next steps include expanding access, developing assessments, and exploring how VR can improve clinical performance and patient safety.
In neuraxial education, the future is immersive and it’s already here.
