Aortic Occlusion in an Adolescent Male Resulting in Intraoperative Multiorgan Failure and Subsequent Death: A Case Report
Jenna N. Littmann, MD, Christa N. Grant, MD, Attending Surgeon Bianca S. Jambhekar, MD, MPH, Ailan Zhang, MD, PhD; Tara M. Doherty, DO
Affiliation: Westchester Medical Center
Published July 3, 2024 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
Brief Summary
We present a case report detailing the challenging management of a healthy teenage male who developed an aortic thrombus that progressed to ischemic multiorgan failure and mortality. Management of this patient included an emergent surgical embolectomy that required intraoperative massive blood transfusion, inotropic support for unstable hemodynamics, and the rare use of emergent, intra-operative continuous hemodialysis for severe hyperkalemia and metabolic acidosis.
Full Case Description
Our patient was a 15-year-old 70 kg male with celiac disease who presented with acute chest, back, and abdominal pain with decreased sensation in his lower extremities. This pain developed while he was exercising, following a week of bloody diarrhea ostensibly attributed to celiac disease. Pertinently, the patient’s mother reported that he had sustained a recent trauma to the abdomen during martial arts practice four weeks prior to admission.
Clinical assessment unveiled a picture of lethargy, pallor, tachypnea, tachycardia, and diaphoresis with lower limb mottling extending caudally from the umbilicus. He had diminished sensory and motor function in his lower extremities and absent femoral and distal pulses. Initial lab results were significant for leukocytosis, mildly elevated creatinine, and low bicarbonate. The pan-computed tomography (CT) scan with contrast revealed an abnormality within the lining of the left ventricle and an approximate 6.5cm abnormality in the aorta (both suspicious for thrombus), concern for ischemia of the spleen, kidneys, and bowel.
He was hemodynamically stable at the time, but as a result of the initial evaluation, he was brought emergently to the operating room (OR) for an exploratory laparotomy with aortic thrombectomy. A cardiologist was present soon after induction of anesthesia to perform a transesophageal echocardiogram which revealed a hyperechoic structure along the left ventricular septal wall consistent with an intraluminal thrombus (Figure 1,2) and mildly depressed left ventricular function. Massive transfusion protocol was instituted early via a rapid transfuser in anticipation of significant blood loss and coagulopathy, and blood product administration was guided with the use of thromboelastogram technology. First intraoperative arterial blood gas revealed pH and potassium values of 7.01 and 5.6mEq/L, respectively, that were initially attempted to be pharmacologically managed. However, the patient’s overall clinical status rapidly deteriorated, and the decision was then made to emergently initiate continuous veno-venous hemodialysis (CVVHD) intraoperatively. Emergent, intraoperative CVVHD is not often utilized in non-liver transplant operations, making this a unique aspect of the anesthetic management in this case report.
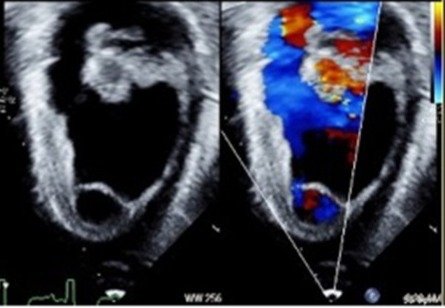
FIGURE 1
A mid-esophageal 2-chamber view of the left ventricle with a hyperechoic structure (likely thrombus) on transesophageal echocardiography.
A total of 22 units packed red blood cells, 15 units of fresh frozen plasma, 7 bags of platelets, and 2 bags (20 units) of cryoprecipitate were administered over the 12-hour surgical period. The combination of hemorrhage, hypotension, metabolic acidosis (with significantly elevated lactate), and hyperkalemia were challenges throughout the case and could not be corrected with maximal interventions in the setting of prolonged lower extremity and multiorgan ischemia.
Intraoperative ultrasound confirmed the presence of a densely adherent thrombus in the supraceliac aorta extending down to and obstructing the branches of celiac and superior mesenteric arteries. Thrombectomy and endarterectomy were performed with primary aortic closure. Frozen section of the specimen (Figure 3) revealed organized (chronic) thrombus. During the initial surgery, there was no obvious bowel necrosis, and therefore no resection was performed. At the completion of surgery, a temporary abdominal wall closure was placed, and the patient was taken to the intensive care unit (ICU) in critical condition. Almost 24 hours later, the patient was taken back to the OR for a subsequent exploratory laparotomy which revealed frankly necrotic small bowel, patchy large bowel necrosis, and no detectable pulses in the infra iliac aorta. Despite the ongoing interventions, these findings were deemed incompatible with life by the surgical team, and the patient’s condition continued to deteriorate. After the patient’s parents were counseled on the findings, the decision was made to pursue comfort measures only. The patient was returned to the ICU and declared deceased later that morning. His parents declined an autopsy.
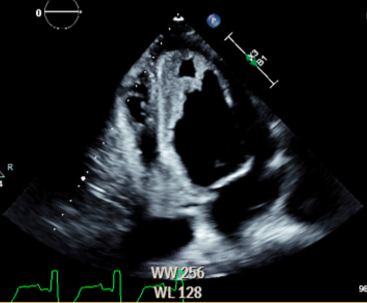
FIGURE 2
Mid-esophageal four chamber view of left ventricle, with hyperechoic structure (likely thrombus) towards the apex.
As the use of intraoperative CVVHD is primarily seen in adult liver transplant literature, the emphasis for this case is the management of acute, refractory hyperkalemia and severe acidosis that necessitated emergent initiation of renal replacement therapy. Our patient’s anticipated hyperkalemia due to lower limb ischemia was unable to be medically managed and caused significant hemodynamic instability. Thus, intraoperative CVVHD was a crucial temporizing measure in this case and required an emergent, multidisciplinary discussion to get the proper equipment prepared in the operating room.
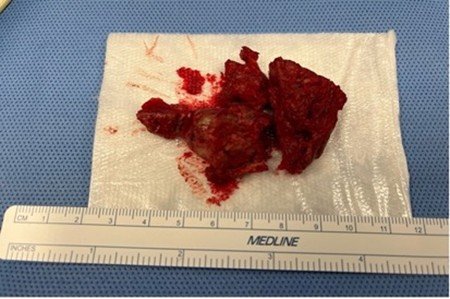
FIGURE 3
Piece of the surgically resected aortic thrombus specimen after embolectomy.
