LMA Management in Neonates and Infants: Clinical Considerations and Case Insights
Charles Kpaheyea, CRNA, Eileen Lyons, MSN, CRNA, Huma Syed Hussain, MD
Published July 3, 2024 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
Each month, the Boston Africa Anesthesia Collaborative (BAAC) hosts grand rounds to promote case-based learning and knowledge exchange in anesthesia practice across resource-limited settings in Liberia. The April session focused on best practices for managing neonates and young patients with a laryngeal mask airway (LMA).
Case Summary
A 10-day-old neonate weighing 3.5 kg was brought to the operating room for excision of a sacrococcygeal teratoma, located at the lower spine near the anus.The vitals were: respiratory rate of 43 breaths per minute, oxygen saturation (SpO₂) of 96%, heart rate of 145 bpm, and a temperature of 36.7°C. Airway assessment showed a small mouth and large tongue, but with a full range of neck motion and normal temporomandibular joint (TMJ) mobility. The patient was classified as ASA I. Laboratory results indicated a hemoglobin level of 15 g/dL and a negative HIV status. Systemically, the patient had no abnormalities, was passing urine normally, and exhibited no signs of jaundice. Preoperative management included administration of Dextrose 5% (100 ml over 2 hours) and Ampicillin 175 mg IV.
A laryngeal mask airway (LMA) size 1 was used. The patient underwent total intravenous anesthesia (TIVA) with supplemental oxygen at 2 L/min. Induction was achieved using Thiopental 20 mg, followed by isoflurane, intravenous paracetamol (PCM) 70 mg, and pentazocine 1 mg. Maintenance anesthesia included isoflurane at 1.6%, PCM 70 mg, and 50 ml of normal saline. Continuous monitoring was maintained throughout the procedure, with all vital signs remaining within 20% of baseline values. The surgery lasted 45 minutes. Postoperatively, the patient was fully awake and transferred to the NICU for continued care.

Figure 1
Mass at lower spine near the anus
LMA Use in Neonates and Young Patients
Laryngeal mask airways have proven to be an effective alternative to endotracheal intubation, especially for short, routine procedures. Their ease of use, lower potential for airway trauma, and favorable safety profile make them particularly appealing in pediatric anesthetic practice.
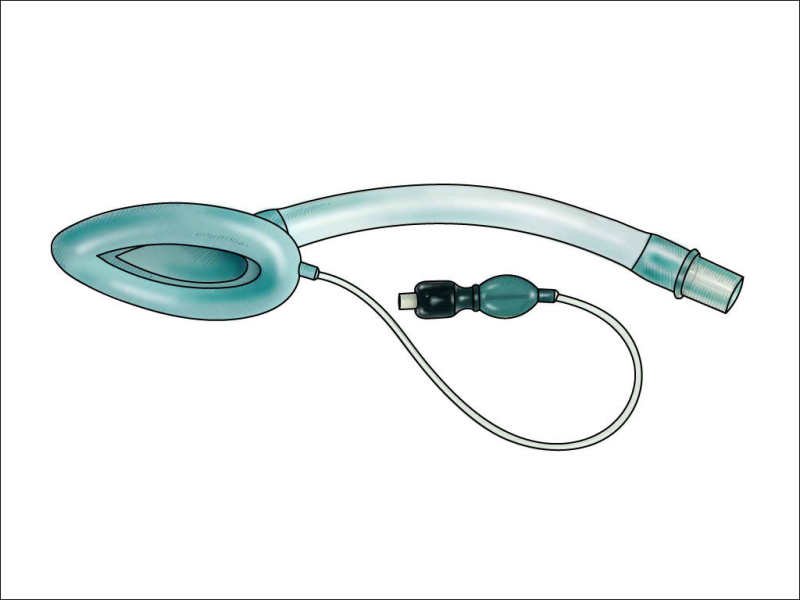
Figure 2
Laryngeal Mask Airway. This illustration is by Scott Dulebohn, MD
Anatomical Considerations in Pediatric Airway Management
Neonates and young children have unique airway anatomy that increases the risk of obstruction. They have a relatively large tongue, a high and anterior larynx (C3–C4), a floppy, omega-shaped epiglottis, and subglottic narrowing at the cricoid cartilage—the narrowest part of their airway. Reduced pharyngeal space further complicates airway management, requiring careful technique and planning.
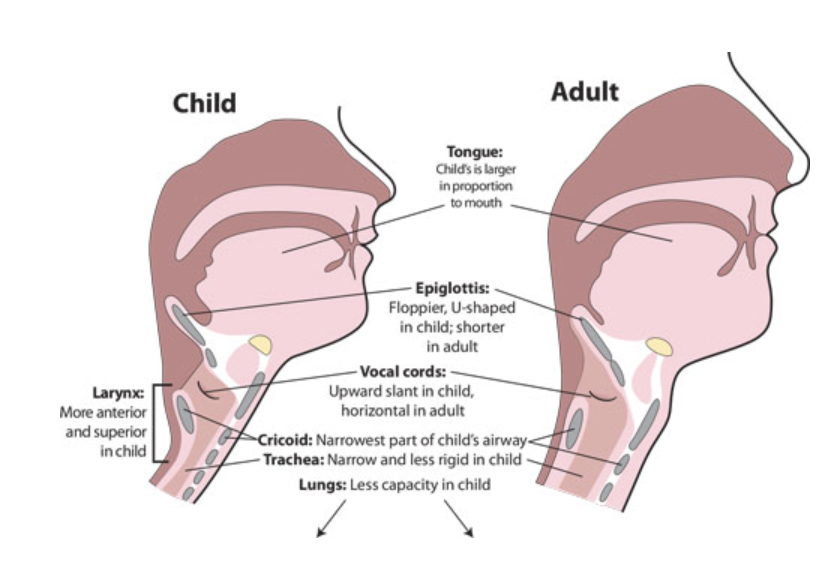
Figure 3
This illustration is from Roberts and Hedges’ clinical procedures in emergency medicine, 6th ed. Saunders: Philadelphia, 2013.
Benefits of LMA Use in Pediatrics
Laryngeal mask airways (LMAs) offer several advantages over endotracheal intubation, particularly in neonates and in resource-limited settings. They are generally easier to insert, reducing the technical challenge and time required for airway management, an important consideration in fragile neonates. LMAs also cause less trauma to airway structures, such as the vocal cords, and are better tolerated, enhancing overall patient comfort. Their use is associated with lower anesthetic requirements and quicker recovery times, making them a valuable option in both elective and emergent neonatal procedures.
Potential Risks and Considerations
While laryngeal mask airways (LMAs) are generally considered safe and effective in neonatal anesthesia, complications can still arise. Improper placement or poor patient selection can lead to airway obstruction or even aspiration. Laryngospasm remains a significant risk, especially if the depth of anesthesia is inadequate during particularly stimulating portions of the procedure. In neonates with abnormal airway anatomy, LMA insertion can be technically challenging. Additionally, excessive cuff pressure may cause mucosal injury, emphasizing the need for careful monitoring. In certain surgical or emergent situations, conversion to endotracheal intubation may become necessary if the LMA fails to provide a secure airway.
Tips for Safe LMA Use in Neonates

REFERENCES
1. Bansal, Satvik Chaitanya et al. “The Laryngeal Mask Airway and Its Use in Neonatal Resuscitation: A Critical Review of Where We Are in 2017/2018.” Neonatology vol. 113,2 (2018): 152-161. doi:10.1159/000481979
2. Disma, Nicola et al. “Airway management in neonates and infants: European Society of Anaesthesiology and Intensive Care and British Journal of Anaesthesia joint guidelines.” European journal of anaesthesiology vol. 41,1 (2024): 3-23. doi:10.1097/EJA.0000000000001928
