Open Repair of Infrarenal Abdominal Aortic Aneurysm in a High-Risk Patient with Cardiovascular and Renal Comorbidities
Sumeeta Kapoor, MD
Published July 3, 2025 | Clinics in Medical Education
Issue 7 | Volume 1 | June 2025
A 66-year-old male (height: 63”, weight: 88 kg, BMI 34, IBW: 56 kg) with no known drug allergies presented for elective open repair of a 6.2 cm infrarenal abdominal aortic aneurysm (AAA), discovered incidentally during evaluation for cellulitis complicated by septic shock and acute renal failure three months prior. His medical history was notable for coronary artery disease (CAD) with PCI to the RCA (May 2024) and LAD (July 2024), preserved left ventricular ejection fraction (64%), and normal functional capacity. Additional comorbidities included type 2 diabetes mellitus (HbA1c 7.5%) on insulin and SGLT2 inhibitors (held pre-op), hypertension, hyperlipidemia, chronic kidney disease (baseline creatinine 2.2, likely stage III–IV), suspected obstructive sleep apnea (undiagnosed, with snoring and witnessed apnea), and prior alcohol use. Medications included aspirin, statin, fibrate, metoprolol, nifedipine, glargine, metformin, losartan, and Plavix (held for 7 days pre-op).
Preoperative Evaluation
Transthoracic echocardiography (April 2025) showed mild mitral regurgitation, severely dilated left atrium, aneurysmal atrial septum without shunt, and normal right ventricular function. Electrocardiogram demonstrated sinus rhythm with left anterior fascicular block and findings consistent with pulmonary disease. Based on cardiac and renal risk, the anesthesia team opted for a combined general and regional approach with advanced intraoperative monitoring.
Anesthesia and Intraoperative Management
A thoracic epidural catheter was placed at the T7–T8 level, with test and loading doses of lidocaine and ropivacaine confirming sensory block to T8. Standard ASA monitors were applied, and a right radial arterial line, right internal jugular central venous line, and an additional 14G PIV were inserted under ultrasound guidance. Monitoring also included TEE and SedLine for depth of anesthesia. The patient was induced with fentanyl, lidocaine, propofol, and rocuronium, and intubated with a 7.5 ETT via McGrath video laryngoscopy. Maintenance included sevoflurane in oxygen/air, with phenylephrine and norepinephrine infusions as needed.
Fluids were restricted before cross-clamping. Renal protection included IV sodium bicarbonate (50 mEq), furosemide (10 mg), and mannitol (7 g) prior to clamping. Heparin was administered with ACT maintained >250 seconds. Aortic cross-clamp time was approximately 65 minutes.
In anticipation of unclamping, the patient received IV albumin, PRBCs, and balanced crystalloids. Ongoing fluid and transfusion therapy was guided by ABGs and TEG analysis, particularly in response to postoperative oozing despite heparin reversal with protamine.
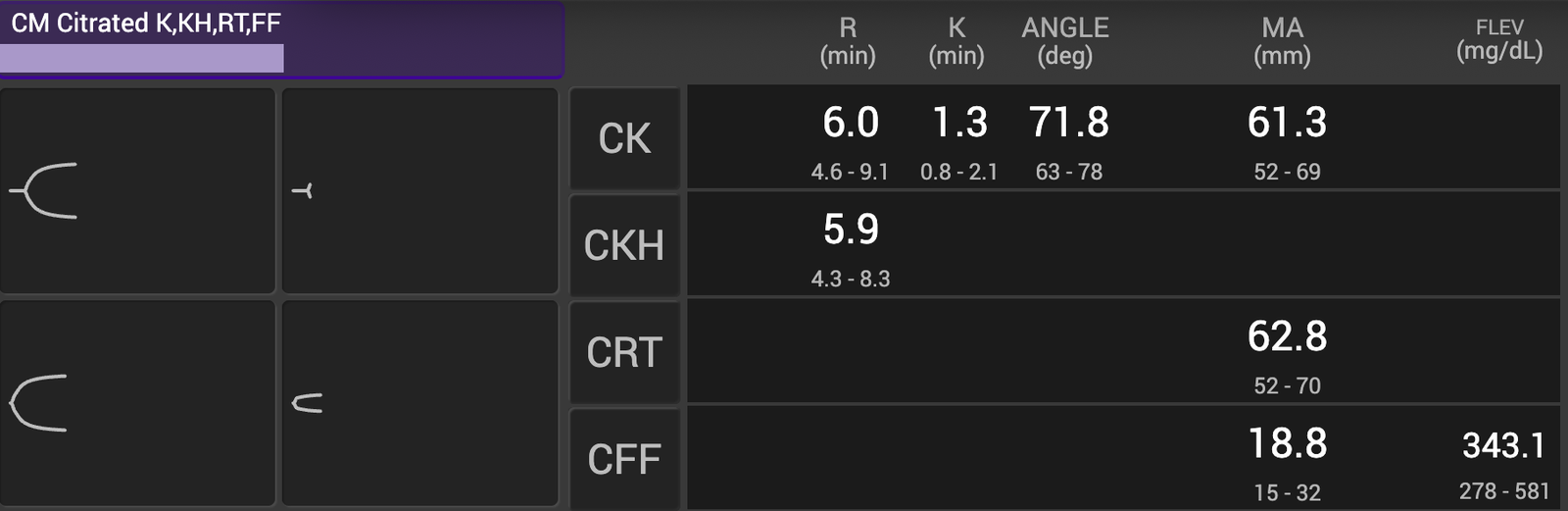
FIGURE 1
First TEG analysis
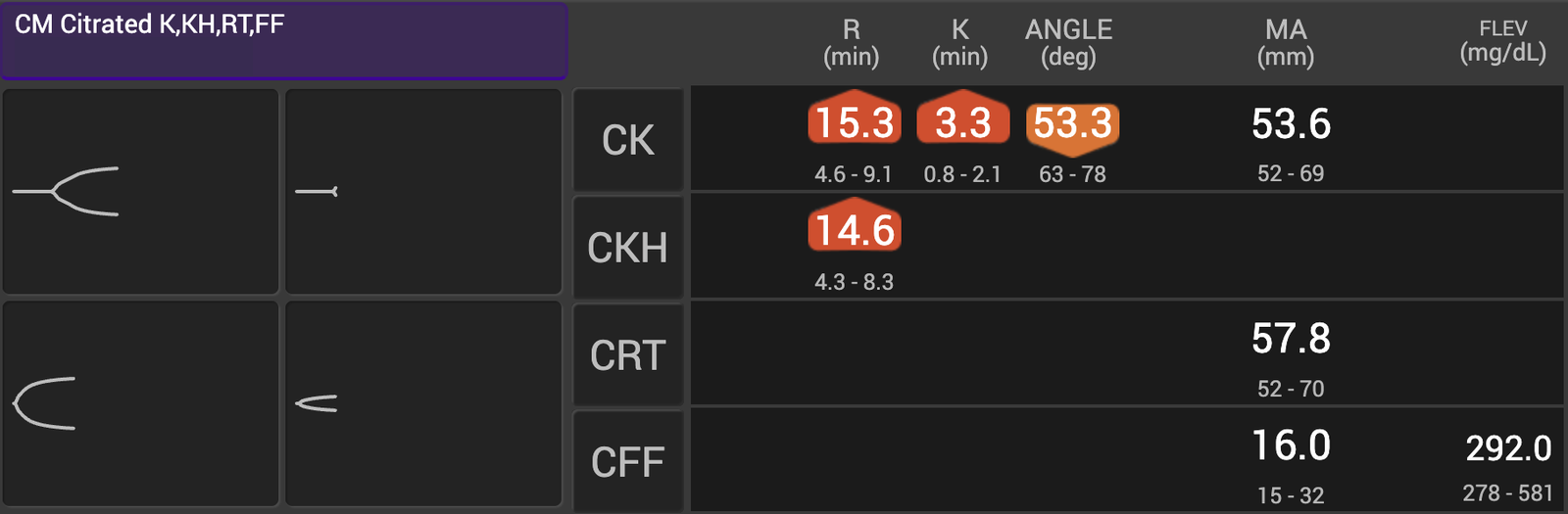
FIGURE 2
Second TEG analysis
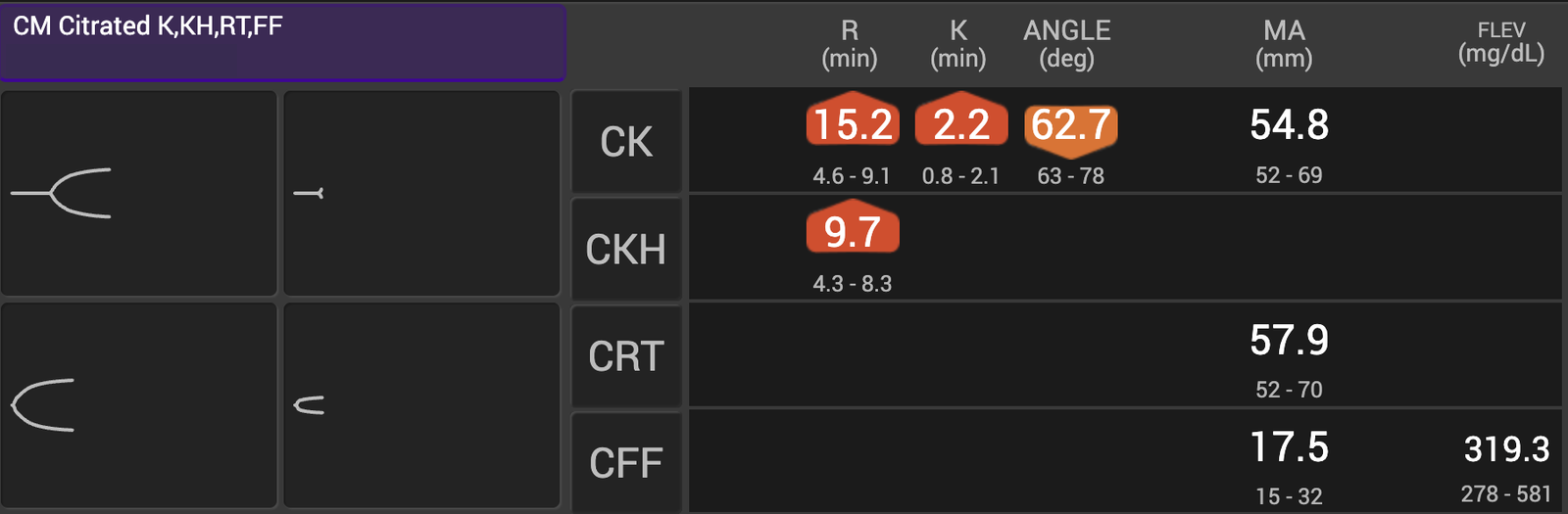
FIGURE 3
Third TEG analysis
Intraoperative Resuscitation and Outcome
Estimated blood loss was approximately 1500 mL. The patient was resuscitated with: 5000 mL of Plasmalyte A, 750 mL of albumin, 700 mL of PRBCs, 330 mL of cell saver blood, 250 mL of platelets, and 200 mL of cryoprecipitate. He was successfully extubated in the operating room after full neuromuscular reversal with sugammadex. Postoperative pain control was managed with epidural infusion and IV analgesics. His recovery was uneventful, and he was discharged home on postoperative day five.
